Here\'s a detailed rewrite of the news article, expanded to a significant word count and enriched with explanatory information.
Title: A Young Life Rescued: 14-Year-Old Dilshad Returns from the Brink of Death with a Revolutionary \'Mechanical Heart\' - A First in India
Introduction: The Whispers of Mortality and the Echo of Hope
In the quiet district of Khorezm, nestled within the vibrant nation of Uzbekistan, a young life hung precariously in the balance. Dilshad, a mere 14 years old, was not battling a fleeting illness or a common ailment. His struggle was far more profound, a silent war waged within the very engine of his existence – his heart. A relentless disease had begun to cripple its pumping power, rendering it incapable of efficiently circulating the vital elixir of life, blood, to his body. The consequences were dire, stealing his vitality, confining him to immobility, and casting a dark shadow of impending mortality over his young shoulders. For weeks, even months, the once energetic teenager found himself tethered to his bed, his world shrinking to the four walls of his room, each breath a testament to his failing cardiac muscle. The chilling prognosis offered by local medical professionals painted a grim picture, a stark reality that threatened to extinguish the bright flame of his youth before it had truly begun to burn. Yet, amidst the despair, a glimmer of hope emerged, a beacon guiding him towards a revolutionary medical intervention that would not only pull him back from the precipice of death but also mark a historic milestone in the annals of Indian medical achievement. Dilshad\'s case, with its profound complexities and its eventual triumphant outcome, has now etched its name in the history books as the first instance in India where a young patient has received a mechanical heart, a testament to the relentless pursuit of medical innovation and the unwavering commitment to saving precious lives.
The Silent Assassin: Understanding Dilshad\'s Predicament
To truly grasp the magnitude of Dilshad\'s ordeal and the significance of his recovery, it is imperative to delve into the nature of the disease that afflicted him. While the original news brief alluded to a condition where his heart couldn\'t pump blood, a deeper exploration reveals the potential underlying pathologies and the devastating impact they have on the cardiovascular system. It is highly probable that Dilshad was suffering from a severe form of Dilated Cardiomyopathy (DCM) or a related condition.
Dilated Cardiomyopathy (DCM) is a serious heart muscle disease where the heart\'s chambers, particularly the left ventricle, become enlarged and stretched, leading to a weakened and inefficient pumping function. In essence, the heart muscle becomes flabby and unable to contract forcefully enough to push blood effectively throughout the body. This inefficiency has a cascade of devastating effects:
* Reduced Cardiac Output: The amount of blood the heart pumps per minute decreases significantly. This means that vital organs like the brain, kidneys, liver, and muscles do not receive enough oxygenated blood to function properly.
* Congestive Heart Failure (CHF): As the heart struggles to pump blood forward, blood begins to back up in the lungs and other parts of the body. This leads to symptoms like shortness of breath (dyspnea), especially during exertion or when lying down, coughing, and swelling in the legs, ankles, and feet (edema).
* Arrhythmias: The enlarged and weakened heart muscle can become electrically unstable, leading to irregular heart rhythms (arrhythmias). These can range from mildly bothersome palpitations to life-threatening ventricular tachycardia or fibrillation.
* Fatigue and Weakness: Due to the insufficient supply of oxygenated blood, patients experience profound fatigue, weakness, and a general lack of energy. Simple activities like walking, talking, or even sitting up can become exhausting.
* Chest Pain: In some cases, reduced blood flow to the heart muscle itself can cause chest pain (angina).
* Organ Damage: Over time, chronic poor blood circulation can lead to damage to vital organs, including kidney failure, liver dysfunction, and cognitive impairment.
In Dilshad\'s case, the description of his condition—where his heart couldn\'t reach the body with blood and his mobility was severely impaired—strongly suggests an advanced stage of heart failure due to a weakened pumping chamber. The inability to walk and talk points to a severe systemic impact, where the lack of blood flow was affecting his neurological function and overall bodily strength.
The initial attempts to manage such a severe condition typically involve aggressive medical therapy. This would include:
* Medications: Diuretics to reduce fluid buildup, ACE inhibitors or ARBs to lower blood pressure and reduce strain on the heart, beta-blockers to slow the heart rate and reduce workload, and sometimes aldosterone antagonists.
* Lifestyle Modifications: Rest, dietary changes (low sodium), and avoidance of strenuous activity.
However, in cases as critical as Dilshad\'s, these medical interventions often prove insufficient. When the heart muscle is too damaged to respond to medication and the risk of imminent death is high, more drastic measures become necessary. For Dilshad, this meant exploring options beyond conventional treatment, leading him to the frontier of cardiac support technology.
The Long and Arduous Journey: From Uzbekistan to India\'s Medical Mecca
The decision to seek treatment abroad is rarely an easy one, especially for a family grappling with the emotional and financial burden of a child\'s critical illness. For Dilshad and his family, this journey was fraught with challenges. The advanced nature of his heart condition likely necessitated specialized medical expertise and advanced technological solutions that may not have been readily available or sophisticated enough in their home country.
The search for a cure would have involved extensive consultations with medical professionals, exploring various treatment avenues, and ultimately identifying India as a beacon of hope. India has emerged as a global leader in healthcare, particularly in complex medical procedures and cardiac surgery, boasting world-class hospitals, highly skilled surgeons, and state-of-the-art technology. The allure of affordable yet high-quality medical care has drawn patients from across the globe, and Dilshad\'s family was no exception.
The logistics of transporting a critically ill child across international borders are complex. It would have involved careful planning, potentially specialized medical escorts, and immense courage and determination from the family. The journey itself, from the initial diagnosis to arriving at a specialized cardiac center in India, would have been a testament to their unwavering love and their refusal to give up on their son.
The Arrival of a Lifeline: The Mechanical Heart - A Technological Marvel
Dilshad\'s arrival in India marked the beginning of a critical phase in his treatment. Upon comprehensive evaluation by a team of leading cardiologists and cardiac surgeons, the severity of his condition was reconfirmed. The traditional options, such as a heart transplant, might have been considered, but factors like donor availability, immunological compatibility, and the patient\'s overall condition often make mechanical support a more immediate and viable solution, especially for younger patients.
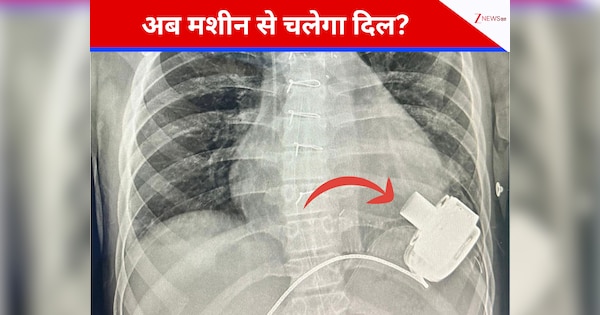
This is where the \"mechanical heart,\" or more accurately, a Ventricular Assist Device (VAD), enters the narrative as Dilshad\'s lifeline. The term \"mechanical heart\" is often used colloquially, but in medical terms, it refers to devices designed to supplement or replace the function of a failing heart. For a young patient like Dilshad, the most likely device implanted would have been a Left Ventricular Assist Device (LVAD).
Understanding the Ventricular Assist Device (VAD):
An LVAD is a sophisticated mechanical pump that is surgically implanted to help a weakened left ventricle pump blood to the rest of the body. The left ventricle is the main pumping chamber of the heart responsible for ejecting oxygenated blood into the aorta, the body\'s largest artery. When it fails, the entire circulatory system suffers.
The components of a typical LVAD system include:
1. The Pump: This is the core of the device, a small, powerful pump that is usually implanted in the chest cavity, often near the apex of the heart. It has an inflow cannula that draws blood from the left ventricle and an outflow cannula that pumps blood into the aorta.
2. The Controller: A small, portable computer that monitors the pump\'s function and adjusts its speed and flow rate. This is typically worn by the patient or kept nearby.
3. The Power Source: Modern LVADs are powered by batteries. The patient usually wears two batteries connected by a cable that passes through the skin (transcutaneous driveline). These batteries provide continuous power to the pump.
4. The Driveline: A crucial component that connects the internal pump to the external controller and batteries. This is a potential site for infection and requires meticulous care.
How an LVAD Works:
In Dilshad\'s case, the LVAD would have been implanted to bypass the failing function of his left ventricle. The device would have taken over the primary task of pumping oxygenated blood from the left ventricle into the aorta. This would have significantly improved blood flow to all the vital organs, alleviating the symptoms of heart failure and preventing further deterioration.
The Surgical Procedure: A Triumph of Skill and Technology
The implantation of an LVAD is a complex and highly specialized surgical procedure, requiring a multidisciplinary team of cardiac surgeons, anesthesiologists, perfusionists, and nurses. The surgery typically involves:
1. Anesthesia and Preparation: The patient is placed under general anesthesia. The chest is opened, usually through a median sternotomy (splitting the breastbone), to access the heart.
2. Cardiopulmonary Bypass: In most cases, the patient is placed on a heart-lung machine (cardiopulmonary bypass). This machine takes over the function of the heart and lungs, circulating and oxygenating the blood while the surgeons operate on the heart.
3. Placement of the Pump: The inflow cannula of the LVAD is meticulously sewn into the wall of the left ventricle. The outflow cannula is then connected to the aorta.
4. Connecting the Driveline: The driveline, which carries power and communication signals, is tunneled through the abdominal wall to exit the skin. This is a critical step to prevent infection.
5. Removal from Bypass: Once the device is fully connected and functioning correctly, the patient is gradually weaned off the cardiopulmonary bypass machine.
6. Closure: The chest is closed, and the patient is transferred to the intensive care unit (ICU) for close monitoring.
The success of such a surgery hinges on the surgeon\'s expertise, the precision of the implantation, and the patient\'s ability to tolerate the procedure. For Dilshad, a 14-year-old, this surgery presented unique challenges, including the size of his anatomy and the potential for growth.
The \"First in India\" Significance: Redefining Possibilities in Pediatric Cardiac Care
The statement that this is a \"first in India\" for a 14-year-old patient receiving a mechanical heart is of paramount importance. It signifies several key advancements:
* Pediatric VAD Expertise: Implanting VADs in children, especially adolescents, is significantly more challenging than in adults. The smaller size of their anatomy, the delicate nature of their blood vessels, and their ongoing growth present unique surgical hurdles. This successful procedure demonstrates a high level of expertise within Indian pediatric cardiac surgery teams.
* Technological Adaptation: Modern VADs are often designed for adult anatomy. Adapting these devices or utilizing specific pediatric models (if available) and ensuring their long-term functionality in a growing child requires specialized knowledge and careful management.
* Resource Availability: The availability of such advanced mechanical circulatory support systems, the skilled personnel to implant and manage them, and the supportive infrastructure in India make it a competitive destination for complex cardiac interventions.
* Pioneering a New Era: This success opens doors for other young patients in India and potentially neighboring countries who may suffer from similar end-stage heart failure. It offers a viable alternative to heart transplantation, which often faces challenges with donor organ availability and long waiting lists. It signifies India\'s capability to provide cutting-edge treatments for even the most complex pediatric cardiac conditions.
Post-Operative Care and the Road to Recovery: A New Lease on Life
The journey does not end with the surgery. Dilshad\'s recovery would have involved an intensive period of post-operative care, rehabilitation, and ongoing management.
* Intensive Care Unit (ICU) Monitoring: In the immediate aftermath of the surgery, Dilshad would have been closely monitored in the ICU for any signs of complications, such as bleeding, infection, or device malfunction. His vital signs, fluid balance, and the function of the LVAD would have been meticulously tracked.
* Medication Management: He would have been placed on a regimen of medications to prevent blood clots (anticoagulants), manage his heart function, and prevent infection. This would require careful monitoring and adjustments based on his response.
* Physical and Occupational Therapy: As his condition stabilized, Dilshad would have begun a comprehensive rehabilitation program. This would include gentle exercises to regain strength, improve stamina, and relearn basic activities of daily living. The goal would be to gradually increase his mobility and independence.
* Driveline Care: The driveline site is a critical area for infection prevention. Dilshad and his family would have received extensive training on how to properly care for the driveline, including sterile dressing changes and monitoring for any signs of redness, swelling, or discharge.
* Psychological Support: Experiencing a life-threatening illness and undergoing such a major surgery can have a significant psychological impact. Dilshad would have benefited from counseling and emotional support to help him cope with the trauma and adjust to his new reality.
* Education and Lifestyle Changes: He and his family would have received thorough education on how to live with the LVAD, including managing the batteries, understanding alarm systems, and recognizing potential complications. Lifestyle modifications, such as dietary changes and avoiding certain activities, would also be emphasized.
The news that Dilshad\'s mobility and ability to walk and talk were restored is a powerful indicator of the LVAD\'s success. It means that the device effectively restored adequate blood flow to his brain and muscles, allowing him to regain his lost functions and return to a semblance of normal life. This is the true measure of the intervention\'s triumph.
The Broader Implications: Advancing Cardiac Care and Offering Hope
Dilshad\'s story is more than just a medical success; it\'s a testament to human resilience, technological progress, and the unwavering dedication of medical professionals. The successful implantation of a mechanical heart in such a young patient in India carries several broader implications:
* Democratizing Advanced Healthcare: This procedure highlights India\'s growing capacity to provide highly specialized and advanced medical treatments that were once the exclusive domain of a few developed nations. It signifies a move towards making such life-saving interventions more accessible.
* Advancements in Pediatric Cardiology: This achievement will undoubtedly spur further research and development in pediatric VAD technology and surgical techniques. It will encourage more centers to develop expertise in this complex field.
* A Beacon of Hope for Similar Cases: Dilshad\'s story will offer immense hope to countless other young patients worldwide suffering from end-stage heart failure, providing them with a tangible possibility of survival and a better quality of life.
* The Future of Mechanical Circulatory Support: As VAD technology continues to evolve, becoming smaller, more efficient, and less invasive, their role in managing heart failure, both as a bridge to transplant and as destination therapy, will only grow. Dilshad\'s case is a pioneering step in this direction for pediatric patients.
Challenges and Future Considerations:
While Dilshad\'s story is overwhelmingly positive, it\'s important to acknowledge the ongoing challenges associated with VAD therapy, especially in pediatric patients:
* Device Longevity and Growth: Ensuring the long-term functionality of the VAD as the child grows is a significant concern. The device may need to be upgraded or replaced as the child matures.
* Infection Risk: The transcutaneous driveline remains a persistent source of potential infection, requiring vigilant care.
* Thromboembolism: The risk of blood clots forming within the device or on its components necessitates lifelong anticoagulation therapy, which itself carries risks of bleeding.
* Psychosocial Adaptation: The long-term psychosocial adjustment for a child living with a mechanical device and the constant need for medical attention can be challenging.
* Cost: While India offers more affordable healthcare than many Western countries, advanced VAD technology and the associated medical care remain expensive, posing a financial burden for many families.
Conclusion: A Heartbeat of Hope for a Brighter Future
Dilshad\'s journey from the brink of death to a life restored is a powerful narrative of courage, medical ingenuity, and the enduring strength of the human spirit. The implantation of a mechanical heart in a 14-year-old in India is not just a medical feat; it is a beacon of hope, illuminating the path for future advancements in pediatric cardiac care. It demonstrates India\'s burgeoning capabilities in tackling the most complex medical challenges and solidifies its position as a global leader in healthcare innovation. As Dilshad embraces his second chance at life, his story serves as a profound reminder that even in the face of overwhelming odds, with the right technology, expertise, and unwavering determination, life can indeed find a way to flourish, beating with a renewed rhythm of hope and possibility. His mechanical heart, a marvel of modern engineering, now pumps not just blood, but also the promise of a brighter future for countless children who may follow in his footsteps.

